Engineering better healthcare
AN ENGINEERING approach towards designing and managing complex systems could transform health and social care, according to a multi-disciplinary report.

Published today by the Royal Academy of Engineering (RAEng), the Academy of Medical Sciences and the Royal College of Physicians, the report proposes a systems-based framework to meet the needs of patients, carers and NHS staff.
The NHS is one of the UK’s largest, most complicated systems, and has faced calls to be overhauled over the past few decades. Pressure to increase efficiencies has increased during this time due to factors such as an increasingly older population with multiple illnesses, real-term reductions in government spending, and the development of new technologies.
Led by the RAEng, “Engineering better care: a systems approach to health and care design and continuous improvement”, outlines the benefits of tackling these issues by taking an engineering approach.
Such a systems-based approach involves working through the implications of each decision upon the project as a whole – by considering the system’s layout, and all elements and interconnections within it.
In the health and care services, four key elements were identified as being vital to improving processes: people, systems, design and risk.
In order to ensure that all four elements are considered in a connected manner, the report’s framework includes project-related questions to be answered in an iterative manner.
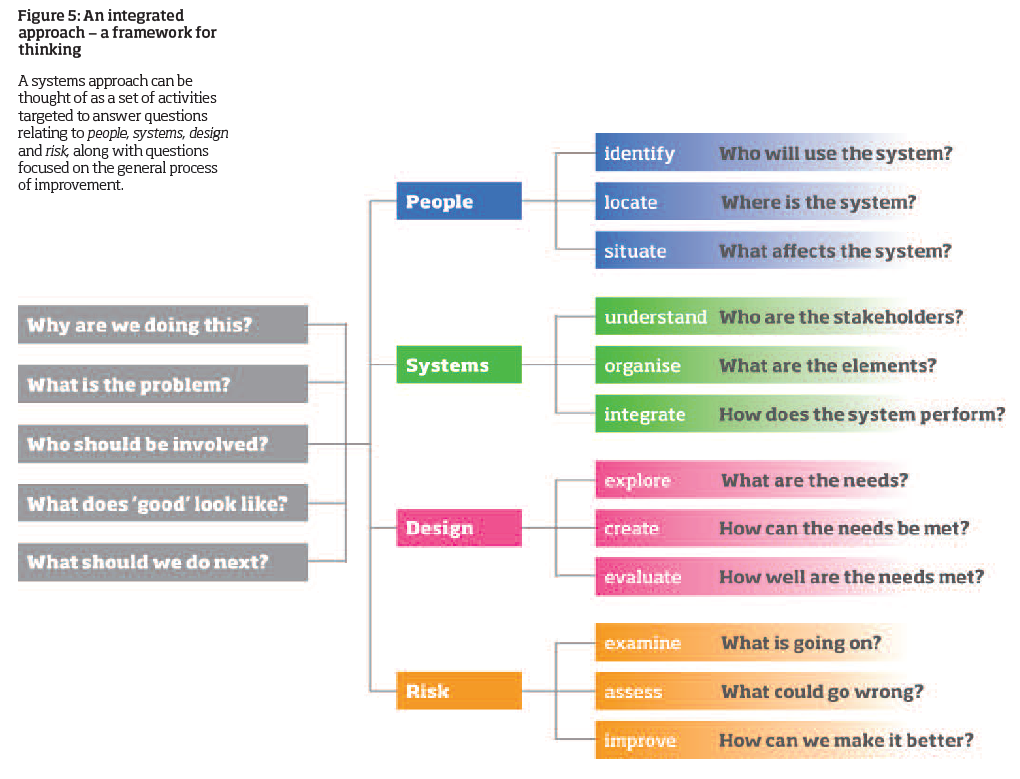
Another key finding of the report was that such ‘common sense’ thinking was in fact far from common in practice.
John Clarkson FREng, who chaired the joint working group producing the report, said: “Making systems that work relies on asking questions to understand the context of the challenge, design a competent system, deliver this system into practice and to sustain its utility and use.
“The power of the simple question in changing the way people think cannot be overestimated – and changing the way that people think changes what they do. Providing them with tools to put into practice their new ways of thinking then transforms what they can achieve.”
The report was based on the findings of a series of RAEng-led workshops involving more than 60 engineers and clinicians. This has led to a network being established of organisation and individuals, who will implement and test the model over the next few years.
For an example of how actively practising the model may look, several examples were given in the report. One such demonstration was a retrospective look at making the design of medication for rheumatoid arthritis and their prescription, delivery and monitoring safer for patients. In this case study, an elderly patient died in April 2000 after her medication’s prescription was accidently increased to a daily dose, rather than weekly.
Asking the framework’s question “what is the problem?”, for example, led to the identification that of 13,000 medicines licensed for use in the UK, the mis-prescribed drug was one of only six to be taken on a weekly basis. Furthermore, more than half of 167 recorded adverse events in almost a decade had been caused by incorrect prescription.
Additional questions identified factors such as information transfer, stakeholders and their needs, assessed “what could go wrong?”, and assessed the system’s performance.
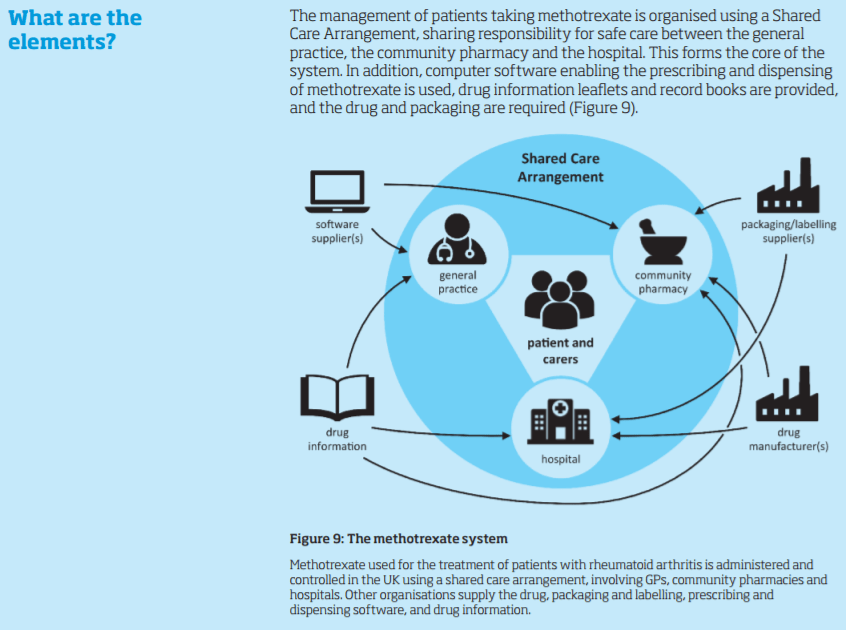
Of the four elements, ‘people’ could be taken into account by improving patient/clinician information, ‘systems’ by considering the wider prescribing, monitoring and medication supply system, ‘design’ by improving protocols and software, and ‘risk’ by acknowledging the patient’s role in taking medicines safely.
Using this real-life systems-based response, measures were then taken to change the supply system of the drug, with the aim of achieving a measurable reduction in patient harm.
Recent Editions
Catch up on the latest news, views and jobs from The Chemical Engineer. Below are the four latest issues. View a wider selection of the archive from within the Magazine section of this site.




